Fabiola Ribeiro loves the sun, the sand and soccer, although probably not in that order. A typical fun-loving Brazilian, she is carefree and easygoing. But her life seems to have turned upside down over the past couple of months, thanks to the zika virus, which has been spreading across Brazil like wildfire. Spread predominantly by mosquitoes, zika is suspected of causing neurological damage in children born to women who were infected during pregnancy. “I did not have mosquitoes in my apartment till about two or three years ago, but now they are a constant menace,” said the 36-year-old from Sao Paulo, who teaches physics at the University of Paulista. “I try to kill every mosquito I find in my home. I put used coffee grounds in vases and clean the drains, but the threat of zika keeps me forever worried.”
Nearly 500km to the east, in the city of Rio de Janeiro, which is getting ready to host the 2016 Olympic Games in August, tension is in the air. With the threat of zika growing by the day, the successful conduct of the games has become a major challenge. “Frankly, I was surprised that such a major outbreak could happen, completely unknown to our doctors and scientists,” said Bruno Dias, who runs Núcleo de Pesquisa de Ciências, a centre that supports research in science. “The unknown nature of zika is the biggest threat. However, little by little, our scientists and doctors are finding clues to understand it better,” he said.
Rogerio Guimaraes, who is an assistant editor of a website specialising in health issues, said a lot of people working with him got affected by dengue last year. “If they got sick with dengue, it could happen with zika, too. Unfortunately, the sanitation condition here is quite pitiful and the government is focused only on mitigation, not prevention,” said Guimaraes, who is from Sao Paulo.
 Uncertain future: Alessandra de Souza Amorim of Campina Grande, Brazil, with her two-month-old son, Samuel, who was born with
microcephaly | Reuters
Uncertain future: Alessandra de Souza Amorim of Campina Grande, Brazil, with her two-month-old son, Samuel, who was born with
microcephaly | Reuters
Many Brazilians complain that the government is not doing enough. “It failed in building sanitary infrastructure and drainage works on time. I really don't know what plans are being made to combat zika, other than the media campaigns,” said Simone Maria Farias, another Sao Paulo resident. As it spreads rapidly across the Americas, zika has become a nightmare not just for Brazil, but for the whole world. The World Health Organisation (WHO) declared it a global public health emergency on February 1.
 Rogerio Guimaraes
Rogerio Guimaraes
The virus was named zika after a forest in Uganda from where it was identified for the first time in 1947. In the local Luganda language, zika means overgrown. The Zika forest, which lies along the highway connecting Uganda's capital Kampala to the Entebbe International Airport, was once home to a major centre for research in tropical mosquito-borne viral diseases. The discovery of the zika virus was accidental. Supported by a grant provided by the Rockefeller Foundation, a group of Ugandan, American and European scientists were working on yellow fever. To verify whether the yellow fever virus infected primates, they put a rhesus monkey in a cage inside the forest so that mosquitoes could bite it. After a few days, the monkey developed a fever, and scientists Alexander Haddow and George Dick isolated a virus from its serum samples. But instead of the yellow fever virus, it turned out to be something not previously seen. And Dick named the virus zika after the forest.
Zika's subsequent spread had been sporadic and slow. The first human infections were reported from Uganda and Tanzania in 1952. Thereafter, its presence was confirmed in parts of Africa and equatorial Asia, including India, Pakistan, Indonesia and Malaysia. Till 2007, there had been only 14 documented zika cases. It all changed in 2007 when the virus hit Yap island, a part of the Federated States of Micronesia, in the western Pacific. More than 70 per cent of the island's population above the age of three was affected, although no casualties were reported. From there, the virus moved to other Pacific islands, with French Polynesia witnessing a major outbreak in 2013-14.
All zika outbreaks occurred in small countries with minuscule populations until 2014, when the virus entered Brazil. There are two theories about zika's Brazilian invasion. The virus could have reached Brazil through football fans who visited the country for the 2014 World Cup. Another theory suggests that the Va’a World Sprints, a canoe race held in Rio de Janeiro, could be the likely culprit as it saw the participation of a large number of Polynesian teams.
DOCTORS IN BRAZIL suspected something was amiss a few months after the World Cup got over on June 13. In many cities that hosted matches, patients complaining of fever, joint pain, rashes and conjunctivitis started flocking to hospitals. Since the cases were mild, doctors thought it could be roseola or fifth disease, but there was no definite diagnosis. Some suspected dengue and some thought polluted water could be behind the symptoms. But after tests ruled out all those possibilities, the disease came to be called doença misteriosa, the mystery disease. Finally, in April 2015, the state lab in Bahia, a state on Brazil's eastern Atlantic coast, tested samples positive for zika. A month later, Brazil's National Reference Laboratory confirmed the diagnosis.
Zika is spread primarily by Aedes mosquitoes, the same genus of mosquito that spreads dengue, chikungunya and yellow fever. Aedes aegypti is the main culprit, while Aedes albopictus is also said to be capable of transmitting the disease. The virus can also spread from a pregnant woman to her child and during blood transfusion. Information about sexual transmission remains inadequate. So far, there are only instances of transmission from men to women. In 2008, Brian Foy, a virus researcher at Colorado State University in the United States, went on a professional trip to Senegal, where he was infected with zika. Upon his return, he passed on the disease to his wife. The second case of zika transmission through sexual contact was reported last month from Dallas. A person who returned from Venezuela is believed to have passed on the virus to his partner. Although research has shown that zika can thrive in saliva and urine samples, there is no evidence yet to prove that it can spread through these bodily fluids.
Zika is quite difficult to track as only one in five people infected with the virus will show any symptoms, although all of them can transmit the disease. “Most people who become infected have no symptoms or have mild symptoms, like acute onset of fever, maculopapular rash [flat, red spots on skin], arthralgia [joint pain] or conjunctivitis,” said Pamela M. Aaltonen, who teaches at Purdue University in Indiana, United States. Some victims may complain of abdominal pain, nausea and diarrhoea. The symptoms appear two to twelve days after a mosquito bite and may last for two to seven days.
 Fabiola Ribeiro
Fabiola Ribeiro
Diagnosis of zika is a major challenge. It can only be confirmed by a laboratory test during the first five days of infection. The average zika incubation time, however, is four to five days, and by that time, the virus would be undetectable. A longer-term assay which is available cross-reacts with antibodies of dengue and chikungunya, making it ineffective in case of an outbreak of all three viruses.
Although the “mystery disease” remained nothing more than a nuisance for the first few months, things began to change quickly. Nearly ten months after the first cases were reported, doctors in cities across northeastern Brazil detected an unusual spike in the number of babies born with misshapen heads. The doctors identified the condition as microcephaly, which was characterised by shrunken head and incomplete brain development. Microcephaly can be caused by a number of conditions like Down Syndrome and other chromosomal disorders. Viral infections like rubella, chicken pox and cytomegalovirus can also cause it. Parasitic diseases like toxoplasmosis, environmental factors, drug/ alcohol abuse, malnutrition, exposure to radiation and lack of oxygen to a baby’s brain while in the womb or at the time of birth have also been proved to cause microcephaly.
Microcephaly can range from mild to severe. In mild cases, the baby will not suffer any lasting damage and will have normal intelligence. But in severe cases, it can cause delays in speech and movement, mental retardation, seizures, hyperactivity, dwarfism, facial distortion and difficulty with coordination and balance. More worryingly, there is no treatment for microcephaly.
The spurt in microcephaly cases in Brazil has been startling. The country reported just 147 cases in 2014. But between January 1, 2015 and February 17, 2016, there have been 3,935 suspected cases, of which 508 have been confirmed.
Doctors and medical researchers now believe that the spike could have been caused by zika, although it has not been proved conclusively. According to the WHO, “evidence that neurological disorders... are linked to zika virus infection remains circumstantial, but a growing body of clinical and epidemiological data points towards a causal role for zika virus.” The prevalence of microcephaly was the most significant factor behind the WHO declaring zika outbreak as a global public health emergency.
The US Centers for Disease Control and Prevention (CDC) on February 10 confirmed the presence of zika virus in the brain tissue of Brazilian infants who had died of microcephaly. It tested tissue samples from two newborns (born at 36 and 38 weeks of gestation) and two foetuses that suffered miscarriage (at 11 and 13 weeks). The samples were from Rio Grande do Norte, a state in the northeastern tip of Brazil. All four mothers had shown symptoms of zika during the first trimester of pregnancy, but they were free of symptoms at the time of delivery/ miscarriage. Tissue samples revealed the presence of zika virus, which belonged to the virus strains isolated from Brazil last year and they showed significant damage to the brain, making it the most likely cause of microcephaly. Test for dengue returned negative. Although these evidences cannot rule out whether there have been cofactors like other maternal infections, this has been the strongest link so far, connecting microcephaly to zika.
Researchers are yet to figure out how zika affects the nervous system. “One possible explanation is that the zika virus, like the cytomegalovirus, attacks stem cells during early brain development, causing general destruction of brain tissue,” said Dr M.K. Sareeshkumar, neurosurgeon at Caritas Hospital, Kottayam, Kerala. “Early loss of stem cells may keep a foetal brain from forming correct architecture.”
According to the WHO, between January 1, 2007 and February 17, 2016, as many as 48 countries and territories have reported local transmission of zika. Of these, only Brazil and French Polynesia have reported increased cases of microcephaly. Another major health concern called Guillain–Barré syndrome (GBS) was reported from Venezuela, Colombia, El Salvador and Suriname. GBS is a rare autoimmune disorder affecting the peripheral nervous system, causing muscle weakness and temporary paralysis. In severe cases, it can cause death in a matter of days. Although the exact cause of GBS has not yet been identified, in nearly two-thirds of the cases, the victims have reported an infectious illness prior to the onset of GBS. It is believed that GBS strikes after the antibodies produced in response to the infection cross-react with peripheral nerve components.
Although GBS is a rare disease with an overall annual incidence of 0.4 to 4 per one lakh people, there appears to be a spike in GBS cases in a few places from where zika outbreak has been reported. For instance, during the French Polynesian outbreak in 2013, the number of GBS cases jumped to 42 from an average of two a year. The recent outbreak in the Americas, too, is heading in the same direction, although scientists are yet to establish a causal link between the two conditions. But experts are worried. “I think we can say that the link between zika and Guillain-Barré looks strong and would be not at all surprising,” said Dr Tom Frieden, director of CDC, in an interview with the Time magazine. “We have seen similar post-infection complications after many different infections, including some that are quite similar to zika. That is a link that's getting stronger.”
In many cities across Latin America, the threat is real and the worry palpable. In Turbo, a modest town in the north coast of Colombia, the number of average GBS cases reported annually has been less than one for the past several years. It all changed after the outbreak of zika. Five cases have been reported in a month's time, from a total population of 60,000. Initially, most people did not even suspect GBS since the incidence was so rare. However, three patients lost their lives in a matter of days. Another one is fighting for his life, while the fifth one has not been able to move her legs for more than ten days now.
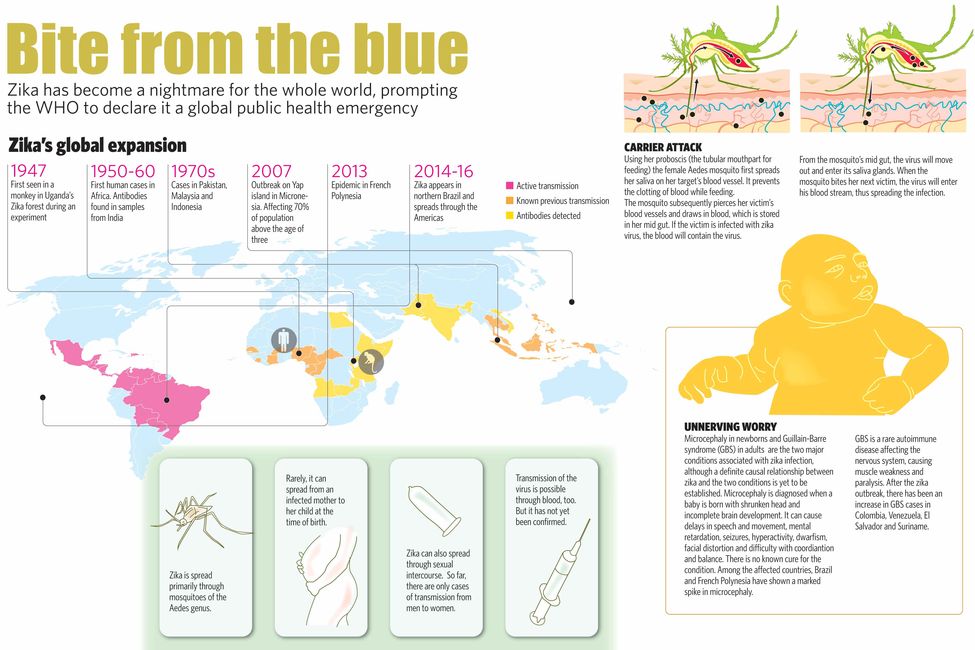 Graphics: N.V. Jose
Graphics: N.V. Jose
HOW PREPARED IS INDIA? With its 1.2 billion population and an army of Aedes aegypti mosquitoes, the possibility of a zika outbreak cannot be ruled out in India. Dengue, which is spread by the same genus of mosquitoes, has already become endemic in India. The number of confirmed dengue cases reported in India has gone up to 84,391 in 2015 (till November 15) from 40,571 in 2014. The number of unreported and undiagnosed cases would be many times higher.
Incidentally, the first zika victim in India was probably Tata Motors. The company's new hatchback, which was launched at the Delhi Auto Expo last month, was named Zica, meaning zippy car. A combination of bad luck and poor research forced the Tatas to find a new name for the car. They have settled on Tiago.
India is no stranger to zika. Even before the infection was officially confirmed in a human being, which happened in 1954 in Nigeria, the presence of zika was confirmed in human samples in India. After the establishment of the Virus Research Centre (which later became the National Institute of Virology) in Pune in 1952, its director, J.A. Kerr, conducted a study on vector-borne viruses, along with K.C. Smithburn of the Rockefeller Foundation and P.B. Gatne, who was the medical officer of Bombay state. The trio collected samples from 38 locations in six states across India to test for 15 vector-borne viruses. It was found that 33 of 196 people tested had antibodies against zika in their blood, although they were not exposed to the virus. The findings of the study were published in the April 1954 issue of the The Journal of Immunology.
“The passive immunity seen in those samples was probably the result of exposure to similar viruses, most likely dengue,” said Dr G. Arunkumar, who heads the Manipal Centre for Virus Research. “In any case, no in-depth analysis of the findings was done at the time and dengue and zika viruses are amazingly similar. So, the past instances of passive immunity are unlikely to help us if we indeed face a zika outbreak,” he said.
“THERE IS NO REASON that zika would not be a threat to India,” said Dr Sajith Kumar, head of the department of infectious diseases at Government Medical College, Kottayam. “Epidemics related to mosquitoes can happen and have happened very easily in India, chikungunya and dengue being two recent examples. Both of these are spread by Aedes mosquitoes, the same vector as that for zika. In fact, zika can perhaps spread faster.” zika also has a tendency to affect larger populations. For instance, during the Yap island outbreak, more than 70 per cent of the population was affected. Kumar said zika could easily affect 10 or 20 per cent of the population during an outbreak. So, if it hits India, we could be seeing victims running into millions, which could overwhelm our health care system.
Dr S.K. Sharma, head of the department of internal medicine at All India Institute of Medical Sciences, New Delhi, said because of the presence of Aedes mosquito, which is a common vector for dengue, chikungunya and zika viruses, there was a real danger of zika infection in India. “The resistance developed by Aedes mosquito to insecticides is another cause for concern. Also, the chances of co-infection of dengue and zika virus and cross-reactivity of blood samples on serological testing make diagnosis difficult,” said Sharma.
 Simone Maria Farias
Simone Maria Farias
Zika being a mild disease, one can fail to spot it. Kumar said we could not say for sure that there were no zika cases in India. “For an average physician, zika and dengue may look the same. Moreover, all physicians say they have seen many dengue cases, which are not so typical. Some of them might have been zika,” he said.
Since so little research was done on zika virus over the years, there are no medicines to treat the infection or vaccines to prevent it. The only method of prevention available is to avoid mosquito bites. As Aedes mosquitoes tend to be active during day when people are at work, prevention is easier said than done. Moreover, the Aedes mosquitoes can live up to three months and it bites people just once a day. They prefer to remain indoors, hiding behind curtains, beneath beds, inside cupboards or even within wardrobes. Routine anti-mosquito measures may not be enough to tackle them. Moreover, Aedes mosquitoes lay eggs in clean, still water, which is found within our surroundings. So, water tanks, air coolers, toilets or even a few drops of water left in a spoon or a bottle cap are potential breeding grounds for them. “Therefore, anti-mosquito measures are not going to be that effective in controlling zika and other diseases spread by Aedes. Anti-larval measures should form the core of our mosquito-control campaigns. We should also realise that repelling measures are not the solution. It only sends mosquitoes from one place to another,” said Kumar.
According to Sharma, since the clinical manifestation of zika might go unnoticed, the efforts should be directed to identify index cases (the first identified case in a group of related cases of a particular communicable disease). It is important to diagnose the infection early and prevent transmission at the community level as well as the environmental level by ensuring sanitation of high quality and a high degree of vector control.
Kumar said the biggest concern for India was the potential link between zika and microcephaly. “Considering our birth and pregnancy rates, if there is a zika outbreak here, it is likely to create a generation of children having problems. The reports about Guillain-Barre syndrome are also worrying. We don’t know whether GBS will affect children. Since it affects the adult brain, it could also affect children’s brain. Although zika infections generally tend to be mild, for whose nervous system is affected, recovery is going to be very difficult,” said Kumar.
Arunkumar, however, has a word of caution. He said zika's association with microcephaly in Brazil was only ecological (meaning, in time and place) and a causal relationship was not yet scientifically established. “It is too early to conclude the casual association of zika virus and microcephaly. We need more data on this from the affected countries. If prospective studies rule out a casual relationship, the infection will not be a major threat to pubic health in India. However, if it turns out to be the opposite, yes, it will be a real threat,” he said.
All the more alarming is the fact that India lack the baseline data on birth prevalence of microcephaly and most neurological conditions like GBS. “This could adversely affect the detection of any increase in prevalence of these conditions and limit our ability for early detection of these trends in the event of widespread transmission of zika,” said Arunkumar.
India, however, has moved quickly within days of the WHO declaring zika to be a global emergency. The National Centre for Disease Control at Delhi and National Institute of Virology at Pune have been identified as laboratories for testing the infection. The Indian Council of Medical Research has been designated to strengthen diagnostic facilities by identifying ten laboratories across the country. India is also in the forefront of global efforts in developing a vaccine to combat zika. Hyderabad-based Bharat Biotech has reportedly developed an anti-zika vaccine, which is all set for clinical trials. However, it could take up to 18 months before the vaccine becomes readily available for public use. That time period is more than enough for the virus to spread to India.
 Weak defence: Children at Ghazipur landfill in east Delhi collecting waste water. Controlling mosquito breeding by adopting hygienic practices is the best way to prevent a zika outbreak in India | AFP
Weak defence: Children at Ghazipur landfill in east Delhi collecting waste water. Controlling mosquito breeding by adopting hygienic practices is the best way to prevent a zika outbreak in India | AFP
What makes India all the more vulnerable is the fact that Indians are avid travellers. “Anything related to travel is likely to reach India faster than any other country as Indians travel a lot and foreigners also visit or transit through the country,” said Kumar. And, this being the Olympic season, there are increased chances of Indians travelling to Rio de Janeiro.
The sexual transmission of zika could be another major challenge for India. With each passing day, more and more cases of zika being spread through sexual intercourse are being suspected. The CDC is investigating 14 such cases and the numbers are only likely to go up. So far, researchers have not been able to confirm how long the virus can stay alive in semen. In the UK, researchers confirmed the presence of the virus in a man's semen 62 days after he fell ill, after a trip to Cook Islands, a part of French Polynesia. “So we are possibly looking at a disease, which has a mixture of features of dengue and HIV,” said Kumar. The CDC at present advises men who have travelled to zika-infected areas to abstain from sex or use condoms for an unspecified period of time. It is difficult to assess the efficacy of such a directive in India, adding to the woes of public health experts.
Eradicating a virus is not an easy task. Despite all advances made by medical science, the only virus we have been able to eradicate is the smallpox virus. The others have not just survived; they are also adapting and spreading across the world. Chikungunya once used to be confined to the French Reunion islands; HIV and ebola were a matter of concern for only a few West African communities; Rift Valley fever was limited to Kenya. Most such infections were geographically limited. But today, people travel a lot and so do viruses, it seems. “Even mosquitoes get transmitted through flights,” said Kumar. Moreover, people have become more susceptible to diseases with changes in lifestyle and dwindling immunity.
“Zika is a bigger menace than any other recent major health scare in terms of its geographical spread,” said Margaret Chan, director-general of the WHO. “Part of the challenge in fighting the virus is that it is so mysterious. We are dealing with a tricky virus, full of uncertainties, so we should be prepared for surprises.”