In the early 1970s, Dr Prakash Narain Tandon, who founded the department of neurosurgery at All India Institute of Medical Sciences, New Delhi, was under a lot of pressure to start operating on his patients. The hospital's first neurosurgical set was yet to arrive and the intensive care unit was not air-conditioned. So, Tandon was ill-equipped to carry out the complex surgeries.
But he had no choice. Very few hospitals in India were equipped to perform complicated neurosurgeries at that time and AIIMS was getting a lot of patients who required surgery. So, armed with a basic equipment set, which was a gift from his mentor, Tandon performed the first surgery. The patient had a huge spinal tumour. No sophisticated imaging techniques were available at that time. So, Tandon planned the surgery, which lasted seven hours, on the basis of an X-ray, and the patient survived.
However, it was nothing compared with the challenges that Tandon faced while performing his third surgery. The 53-year-old patient had brain tumour and there was no way Tandon could ascertain its exact location, size or nature. He opened the patient's skull to find that the tumour had spread to every corner of the brain. After nine and a half hours, Tandon was still operating when his senior colleague, Dr Baldev Singh, asked him to stop. “How could I stop at that point? The decision was a difficult one as the patient could have died of trauma caused by such a long surgery,” says Tandon. “But I told him [Singh] that I had to finish my work. If the patient died on the table, I would curse myself that I didn’t listen to you but if he died of tumour, I would not be able to forgive myself.”
It took him another six hours to finish the surgery. The next morning, the patient regained consciousness, but soon passed out. “I realised that it was because of the heat in the ICU. I sponged him and sat beside him for another twelve hours,” says Tandon. “For a young surgeon, losing a patient could mean the end of his career. Thankfully, he survived the surgery and lived for many more years.”
When Tandon talks about the premier institute today, he feels nostalgic. “There was no OPD [outpatient department]. We used to work out of the dormitory of the nurses’ hostel,” he says.
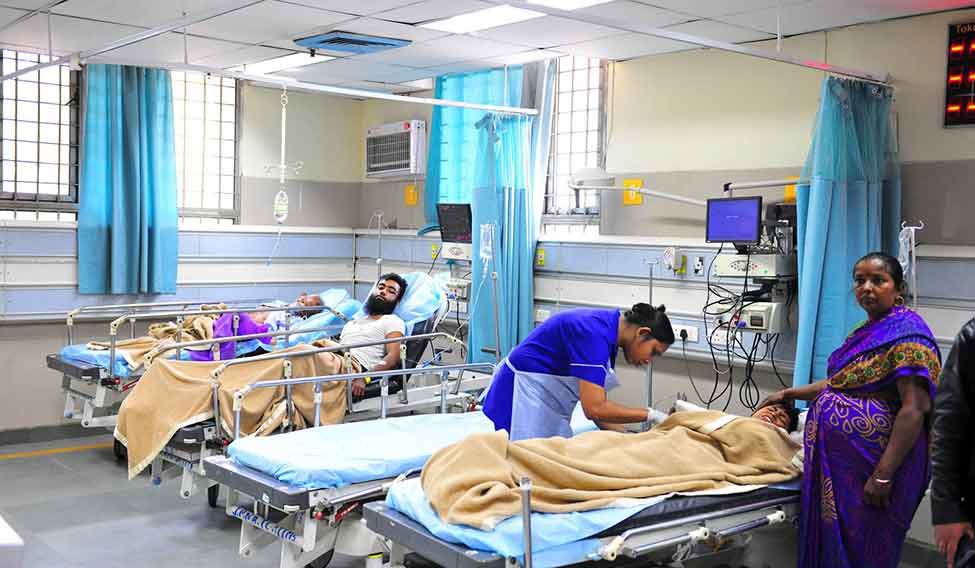 Growing demand: Patients inside AIIMS trauma centre. The hospital plans to add 3,500 more beds to its existing 2,500 by the end of next year | Aayush Goel
Growing demand: Patients inside AIIMS trauma centre. The hospital plans to add 3,500 more beds to its existing 2,500 by the end of next year | Aayush Goel
Founded in 1956, the institute was the brainchild of prime minister Jawaharlal Nehru and health minister Rajkumari Amrit Kaur, whose dream was to bring the country's best talents under one roof. The seed money—one million pound sterling—was given as a grant by the government of New Zealand. The health ministry formed a team to invite Indian doctors working around the world to join the institute. And they came.
The enthusiasm among the newly opened hospital doctors was visible even on the road near the Safdarjung Hospital, which is located right across the AIIMS. “The doctors used to stand on the road outside Safdarjung Hospital to plead with the patients to come to AIIMS instead of consulting a Safdarjung doctor,” says Dr B.N. Tandon, gastroenterologist who joined the institute as a research fellow in 1961.
The doctors were dedicated to building a world-class hospital and invested a lot of time in it. They spent their mornings in the clinic, afternoons were reserved for teaching, and evenings for research at the laboratories. “The institute was supposed to produce world-class doctors, medical faculty and research,” says Tandon.
Almost 60 years later, the routine hasn't changed much for the doctors. Take Dr Kapil Dev Soni, who looks after the intensive care unit at AIIMS trauma centre, for instance. His day starts at 8am and continues till 7pm, and even after that, he is just a phone call away from his patients. On weekends, Soni works on his research project—to decode the complexities of abdominal injuries. “Most critically-ill patients come to the ICU. These patients come with either multiple injuries or severe infections or both. The mortality is high. So, my job is emotionally and physically exhausting,” says Soni, who still prefers AIIMS over private hospitals. “The institute allows me to serve the poor and critically-ill patients. It is a state-of-the-art facility. Besides, it allows me to pursue my academic and research interests.”
The institute, which initially had just 80 faculty members, today has a staff strength of 650. By the end of next year, it would add 3,500 more beds to its existing 2,500. It would also have a separate 200-bed surgical wing with 12 operation theatres, a mother and child centre, and a new OPD block to accommodate the growing patient flow. “The new digitisation drive has helped the patients tremendously,” says M.C. Misra, director of AIIMS. “We are working towards bringing down the waiting time for medical procedures and make the process as smooth as possible for the 3.5 million patients who come to AIIMS for treatment every year.”