In September 2017, Lt Col Amar Dehal of Rashtriya Rifles was shot twice during a terrorist attack in Kashmir’s Shopian district. One bullet hit him in the head―it went in through the right lobe and got lodged in the left; the other scraped through his abdomen. A physically fit, tall and broad-chested Dehal was suddenly bed-ridden and on life support. The entry wound in his skull was closed with an acrylic plate, but the left side remained pulpy to the touch. For eight months, the camera-friendly, guitar-loving 35-year-old was in a coma. Once he was out of it, he was wheelchair-bound, unable to perform the most basic tasks.
This November 1, at the neurorehabilitation department of Kokilaben Dhirubhai Ambani hospital in Mumbai, a cheerful Dehal, assisted by a robot, walked for the very first time in five years. It was “as if he was a baby who was just discovering the pleasures of stretching his legs and learning how to walk from the very beginning,” says his wife Sheela, also a lieutenant colonel. She is on a long hiatus to be with her husband.
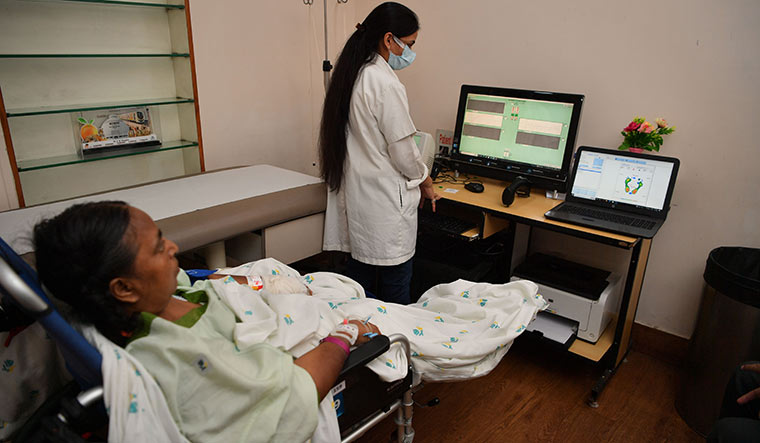
Dehal was seen moving his lower limbs to and fro on a Locomat―a moving mat similar to an automated treadmill―wherein a robotic exoskeleton provides guidance and bodyweight support to facilitate intensive walking training and physiological gait rehabilitation for severely impaired neurological patients. For the next 10 days thereafter, he walked close to 7,000 steps. Egging him on was a video game-enabled screen that rewarded him with jackpots on achieving his milestones. “This advanced technology is akin to magic for us,” says Sheela. “[It] helped him take his first steps into recovery with a hope that one day, very soon, he would be able to walk on his own.” For those who undergo severe mental trauma or stroke, gait disturbance is one of its major consequences. It leads to impaired walking ability owing to loss of signal from specific locomotor centres in the forebrain and command cells in the lower brainstem, which activate the neural networks in the spinal cord. “That’s when technology in the form of artificial intelligence steps in,” says Dr Abhishek Srivastava, director of physical medicine and rehabilitation at the hospital. “This robot-assisted therapy enables the patient achieve balance and gait, which is one of the foremost goals of neurorehabilitation.” The robot interacts with the patient’s limbs during movement training and gives a bio feedback on how much power he generates in a day, explains Srivastava. Its augmented feedback keeps challenging the patient after each level is met. “In case of Dehal, there was significant weakness and stiffness of the body on all four limbs and so with the Locomat, the goal is to make him suitable enough for basic mobility and independence, which will happen soon,” he adds. “In the absence of the Locomat Pro, which is the latest upgraded version installed recently, we would use manual therapy on a patient like this and it would take years to really see positive outcomes.” In the last two years, the desperation and urgency required to tackle Covid-19 led to a “mind-boggling” amount of research and innovation in health care technology, say experts. And two years on, all that hard work has paid off in the form of newer technologies and upgraded versions of existing ones in diverse branches of medicine, especially in those that got sidelined during the pandemic but had to be made future-ready. And, hospitals have embraced these with open arms, in a bid to be in tune with the evolving tech-based mode of care and treatment and also to beef up and streamline their own existing structures and processes as mandated by a post Covid world. “Also, post Covid, with enhanced focus on health care, there was a full-fledged attempt to bring down the cost of all these technologies by huge margins so as to ensure that every branch of medicine remains at par with the best in the world and advanced treatments become affordable, especially in smaller towns and cities,” says Dr Somashekhar S.P., global director of Aster International Institute of Oncology.
Take, for instance, the case of a 12-year-old girl who came to Mumbai’s Jaslok hospital with a severe headache and partial paralysis of her left hand and leg. Investigation revealed a cavernoma―a cluster of abnormal blood vessels―and a bleed in the right side of the brain. The lesion was located in the motor cortex that controls her left hand and leg movements. A surgery was essential but not easy as absolute precision was required to approach the deep-seated tumour and even a millimetre here or there could result in paralysis.
In came the neuronavigation system, a brain GPS of sorts that has been a routine in neurosurgeries in the US but not so prevalent in India. Before opening the skull, the lesion’s location with relation to the scalp was mapped using the neuronavigation system. This helped the doctor to zero in on its location and cut open only that part of the skull. Also, a strip electrode was used to stimulate the part of the brain that controls the left hand and leg movements. “This helped us to understand exactly the relation of the lesion with respect to the area of the brain that controlled hand and leg movements,” says neurosurgeon Dr Sudheer Ambekar. “Then, the lesion was resected using microsurgical techniques while preserving the area of the brain and fibres that controlled hand and leg movements. This sort of precision was unthinkable of earlier. Although neuronavigation in itself is not new, as of today it has been super sophisticated to suit the minutest, deep-seated tumour removal. And, the fact that hospitals are now at the forefront of bringing all these technologies at the earliest is a welcome change.”
While a surgeon’s experience and expertise matter, the technology acts as the ultimate guide tool, says Ambekar. “The chances of going wrong are very less and post-operation recovery is super fast because no other tissue has been touched or damaged in the process,” he says. The girl―all recovered and strong―is back in school. In the case of patients suffering from Parkinson’s, epilepsy and tremors, existing technology became further sophisticated with the launch of the SenSight directional lead system. It helps surgeons pick brain signals and optimise stimulation to each patient’s specific symptoms and anatomy. At Aster CMI hospital, Bengaluru, the device was first used on a 60-year-old who has had Parkinson’s for eight years. “This method is easy to program, accurate and effective,” says Dr Ravi Gopal Varma, director, Aster Global Institute of Neurosciences and Lead Neurosciences. “We are the first to use the device in India. We are able to see how the new stimulation settings are affecting the patients in real time.”
Another aspect that has undergone a remarkable change post Covid is the application of robot-assisted minimally invasive surgeries across specialties, from neurology and orthopaedics to oncology and now even gynaecology. Again, this has a lot to do with low-cost, made in India robotic machines that have enabled even smaller hospitals to induct technology into their surgeries, says Somashekhar.
When Apollo Hospitals, Bengaluru, launched the country’s first dedicated robot-assisted cardiac surgery unit in 2019, it was a milestone in the history of cardiovascular surgery. Patients with complex cardiac disease were offered minimally invasive cardiac surgery with the advanced da Vinci Xi, the world’s first FDA-approved robotic surgical system manufactured by US-based Intuitive Surgical. The most recent one offered by Indraprastha Apollo Hospitals, Delhi, is the robot-assisted total arterial bypass surgery for triple vessel coronary artery disease. Two years ago, when Ashok Joshi, a septuagenerian, underwent robotic prostatectomy―a keyhole surgery for prostate cancer―carried out via da Vinci under the supervision of Dr Santoshi Nagaonkar from Hinduja hospital, he knew he was taking a chance. Da Vinci Xi performed the entire surgery during which its arms could easily navigate any nook and corner of Joshi’s pelvic area without disturbing the minutest of arteries, veins or the tiny blood vessels. But it all turned out to be “super expensive”for him as he had to shell out close to Rs3 lakh more than the conventional surgery.
Cut to 2022, and there is Mantra, the desi rival to the da Vinci which is alike in precision and performance with equally promising post-surgical outcomes but at less than half the cost. “The Mantra, launched this September, was developed by Gurugram-based SS Innovations (SSI). “The da Vinci system costs between 06 crore and Rs15 crore, while Mantra is in the Rs4 crore to Rs5 crore bracket and its operation and maintenance cost is one fourth of the da Vinci robotic system,” says Dr Sudhir Srivastava, chief of SSI. This again was possible only because of Covid, says Somashekhar. “At that time, we wanted to do non-contact surgeries, and while it became commonplace in the US, only a few hospitals in India were undertaking it,” he says. “That’s why in terms of health care tech, this has been a breakthrough period because an unprecedented amount of tech transfer happened during this time.” It has also brought down the costs of tests and drugs, especially in oncology, he says. “One example is ovarian cancer in which HRT (Hormone Replacement Therapy) testing is now being done [here] at one tenth of the cost [in the US] and the drug brought by an Indian pharma company is also available at a fraction (Rs50,000) of the cost of its US counterpart (Rs2.9 lakh),” he says. As Rinku Mavani, business partner-sales, Fortis Hospitals, Mumbai, says, rapid adoption of value-based care models and increasing application of technology and automation across the health care industry, prompted by the pandemic, will continue to be the key driver for health care in the long term.
What we are witnessing is a major shift in the health care sector, especially with the coming in of IoMT―internet of medical things. With medical devices, data and equipment connected to the internet, we have moved into an era of continuous digitised health care, enabling real-time monitoring of medical data, of patients’ vitals and more. From using artificial intelligence for early detection and accuracy of diagnosis and for administrative tasks such as scheduling patient appointments, processes have become much more leaner, accurate, faster and precise, say experts. In a research paper published in the journal of National Center for Biotechnology Information this March, Mukesh Chandra from the department of production and engineering at BIT in Jharkhand, writes, “Covid-19 played a vital role in the improvement and development of medical and health care facilities, and in service delivery.” He identifies digital technologies and industry 4.0 tools such as 3D printing, artificial intelligence, cloud computing, autonomous robots, biosensors, internet of things, virtual reality and holography that are already changing the country’s medical landscape. At Kokilaben Dhirubhai Ambani hospital, Dr Varsha Vadera, head of laboratory medicine and advanced diagnostics, walks us through the hospital’s total lab automation―an integrated system wherein specimens are processed, tested and even stored with minimal user intervention. “It includes biochemistry, immunology, haematology, and serology,” she explains. “In the total lab automation, once the samples are received, they are put in a bulk loader which segregates all samples as per specialised departments and then what follows is the centrifugation. This is being done to reduce the overall turnaround time, to be able to perform tests 24x7 and with minimum human error.” Hospitals across the country have also had a moment of introspection, triggered by the pandemic, prompting them to bring in technologies that will help in easing their day-to-day operations and in turn lead to customer satisfaction. “Bombay Hospital has been at the forefront of computerisation as well as technology at all our group hospitals―Mumbai, Indore and Jaipur (under construction),” says Dr Rajkumar V. Patil, director, medical services, Bombay Hospitals. “We are in the process of using artificial intelligence for various patient as well as equipment-related applications at our Mumbai as well as Indore units.” Manipal hospital in Bengaluru has already initiated a chatbot and conversational AI to improve patient interactions. “Patients and their family can reach out to us over WhatsApp and the chatbot can handle a fair bit of preliminary queries,” says Dilip Jose, MD and CEO, Manipal hospital, Bengaluru. “We have already launched the first version and we continue to add further features to it. The next level is to enable it to make payments…. By automating communication on WhatsApp with the help of chatbot, we increase ease of access for the consumers.” Recently, the hospital also started using wearables to monitor patients remotely long after they have been discharged from the hospital. “This helps us in ensuring a highly cost-effective, AI-driven solution for detection, monitoring and rehabilitation in a home setting, far from the hospital,” says Jose. “Initially, we have selected two therapeutic areas: joint replacement and post-cardiac intervention like an angioplasty. For instance, post total knee replacement, a patient has to exercise and walk and post angioplasty, a patient has to follow a certain regime. We provide them with Fitbits and ask them to download an app so that we are able to track the patient’s movements and get the basic vitals which are then displayed onto a dashboard for the doctors to examine.”Manipal provides its patients with Fitbits for a nominal rental fee.
Pankaj Malhotra, 51, underwent a coronary angioplasty on September 26 and has been on the hospital’s radar even after discharge. “They put in a stent due to a 95 per cent blockage; [I had] no history of cardiac issues,” he says. “Thankfully, I had reached the hospital within the golden hour. Before discharge, I had the patient care team come to me and counsel me on the wearable technology related to my post cardiac rehabilitation…. This tech was to be in sync with the Manipal app which would send me reminders about my medicine time and dosage and a feedback if at all I adhered to it or not. Till date, they have been in regular contact via reminders and followup calls at least thrice a week.”
Aster, too, plans to focus more on data collection through wearables, says Dr Azad Moopen. “Aster DM Healthcare has always ensured that it stays ahead in technology, and introduced the Metaverse in Medcare hospital in UAE and India’s first deep brain stimulation surgery using SenSight directional lead system,” says Moopen, managing director, Aster DM Healthcare. “We successfully conducted remote ICU monitoring of patients during Covid, which is one of the trends that could become mainstream in the future.” Another technology that the group is working on is a Secure Federated Learning Platform (SFLP) to study health data. “[We] launched an AI Lab in association with the Indian Institute of Science (IISc), Bengaluru,” he says. “This will build cutting edge AI initiatives in health care and bridge the gap between clinical medicine and technology by training health care professionals.” Technology has rekindled hope in Dehal, making him believe that very soon he would be able to “at least go to the bathroom” by himself. And, he sees his trauma in a different light. “What if the bullet had passed a few centimetres below? I would have been paralysed for my entire life then,” he says. “God saved me. I’m meant to contribute towards bigger things. I want to go back to my regiment and continue fighting for the country.”
Reversal of diabetes
We have the largest number of people with type 1 diabetes and second largest with type 2 diabetes. Post Covid, we saw an exponential rise in people with type 2 diabetes. This has happened mainly because of the huge lifestyle disruption in the last two years.
The best part is that type 2 diabetes can be reversed. A woman with more than 80cm of waist circumference or a man with more than 90cm of waist circumference should be screened for diabetes after the age of 20 in India.
Traditionally, people in India got diabetes almost two decades before the western world. So if they got it in their 60s, we would get it in our 40s. But now we are seeing people in their 20s getting it. This is because of the fast food culture. There has been an increase in diet high in carbohydrates and fats, but low in proteins. Exercise has gone down.
Type 2 diabetes in the younger generation can be reversed. Eat less, no more than 800-1,000 calories per day. Reduce carbs, increase proteins. Exercise―8,000-10,000 steps a day; suryanamaskar and sit-ups are very effective. Sleep for no less than seven hours. Monitor your sugar levels and blood pressure regularly. Try to keep the HbA1c level below 6.5, keep blood pressure below 130/80 and LDL cholesterol below 70.
―Dr Shashank Joshi, diabetologist, Lilavati hospital, Mumbai
* YOU NEED TO KNOW *
Children’s health
In the past few months, doctors say they have been observing issues related to multiple viral and bacterial infections, obesity, antimicrobial resistance and early pubertal changes among children. “We are seeing many girls coming to us with early features of puberty, which is a process wherein first the breast development happens; menstruation is the final stage of puberty,” says Dr Sudha Rao, head of paediatric medicine at Mumbai's Bai Jerbai Wadia Hospital for Children. “The onset of puberty is usually seen in girls above the age of eight. But post pandemic, we are seeing girls come to us as early as six and seven years. If it happens early, then menses also start early.”
In girls, menarche occurring at eight and a half or nine is considered to be very early and abnormal. Ideally, menses should start around the age of 12, says Rao. She attributes early menarche to children putting on weight during lockdown. Children in the west, she says, are obese because they consume more carbs than protein as food rich in carbohydrates is cheaper. “And, obese girls [there] hit puberty as early as the age of six,” says Rao. “That's exactly what's happening here as well.”
Obesity, say doctors, is the number one negative outcome of Covid among children. So is antimicrobial resistance as they were given antibiotic pills for any and every viral infection in the past two years. Now they are reporting lower respiratory tract infections for which first-line antibiotics do not work.
In this new normal, doctors advise parents to spend more time with their children to help them cope with physical, emotional and psychological pressures that accompany a changing milieu.
* YOU NEED TO KNOW *
Covid and emerging variants
Tremendous evolution has been seen in the case of SARS-CoV-2. It will keep emerging until the spread is stopped. However, the type and behaviour of the emerging variant cannot be predicted at this point. Majority of SARS-CoV-2 variants of concern had more or less similar type of behaviour―increased transmissibility and immune-escape potential. A person with comorbidity is more likely to get infected. Vaccination will help lower the risk of severe disease, hospitalisation and mortality. Besides this, hand hygiene, masking and avoiding crowded places should be followed.
Across the globe, news of a high number of Covid cases is emerging. As of November 12, the World Health Organization data on Covid-19 reported close to 15 lakh cases in one week alone. But India has not seen a surge in cases, with only 6,445 cases newly reported in a week. A surge cannot be predicted at this point in time.
We are presently seeing the XBB subvariant. XBB is a recombinant of BA.2.10.1 and BA.2.75, both of which are sublineages of BA.2; BQ.1 is a sublineage of BA.5, both are the Omicron variants. Although these variants had caused an increase in Covid cases, there is no epidemiological evidence that these subvariants pose a higher risk than other Omicron variants.
Everyone should opt for booster shots, including children, because many studies have proven that the natural or vaccine-induced immunity wanes over six months. Winter is being linked to the possible emergence of a new wave, but there is no direct evidence available to prove that.
―Dr Pragya Yadav, scientist, ICMR-National Institute of Virology, Pune
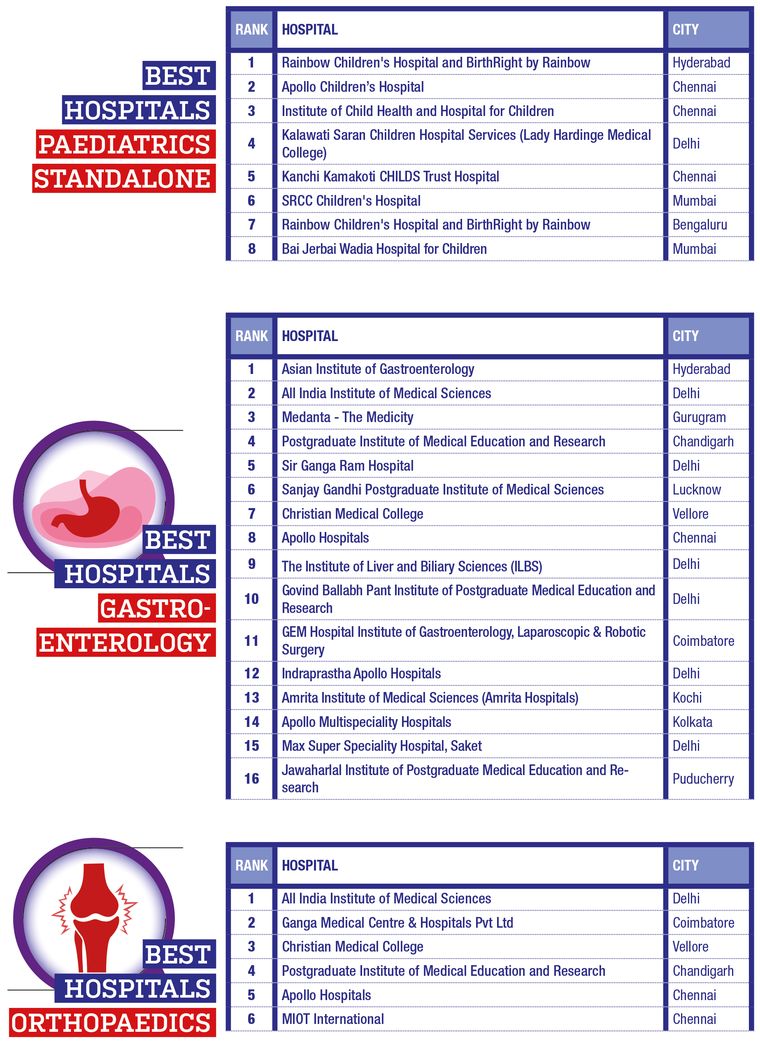
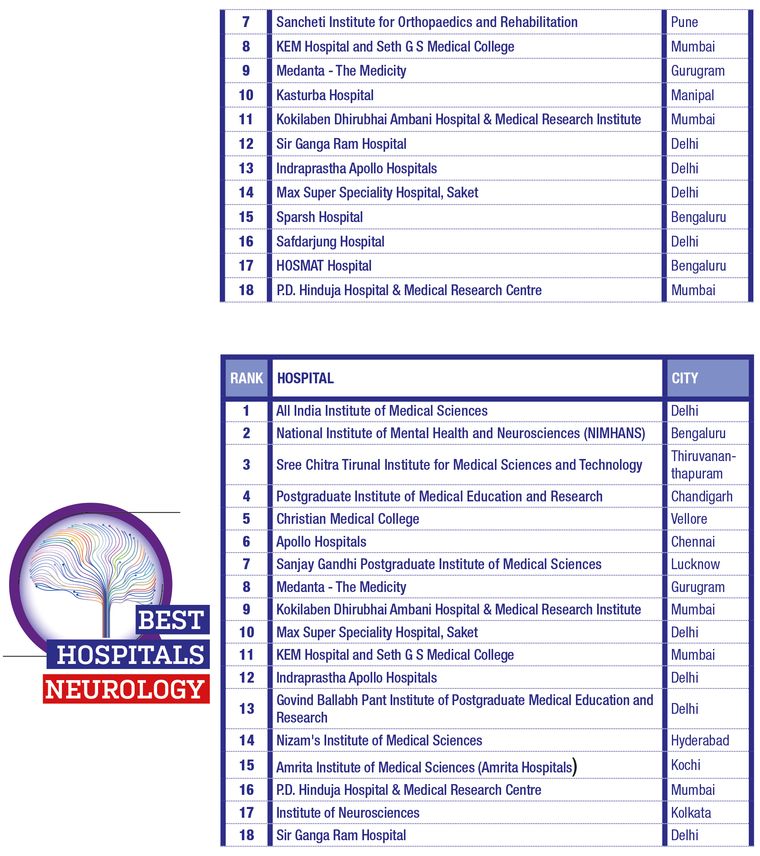
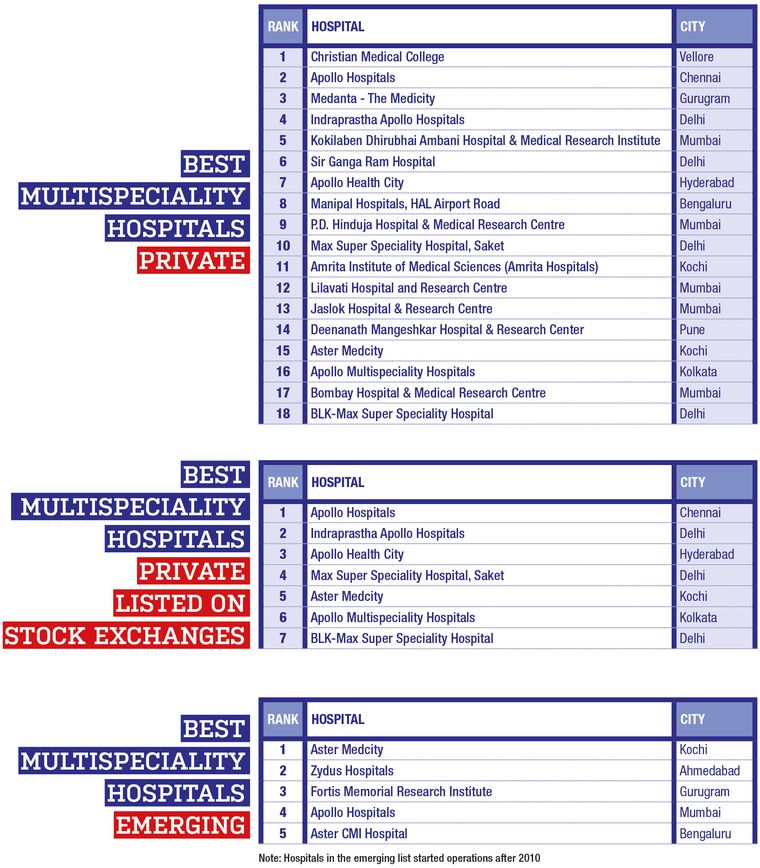
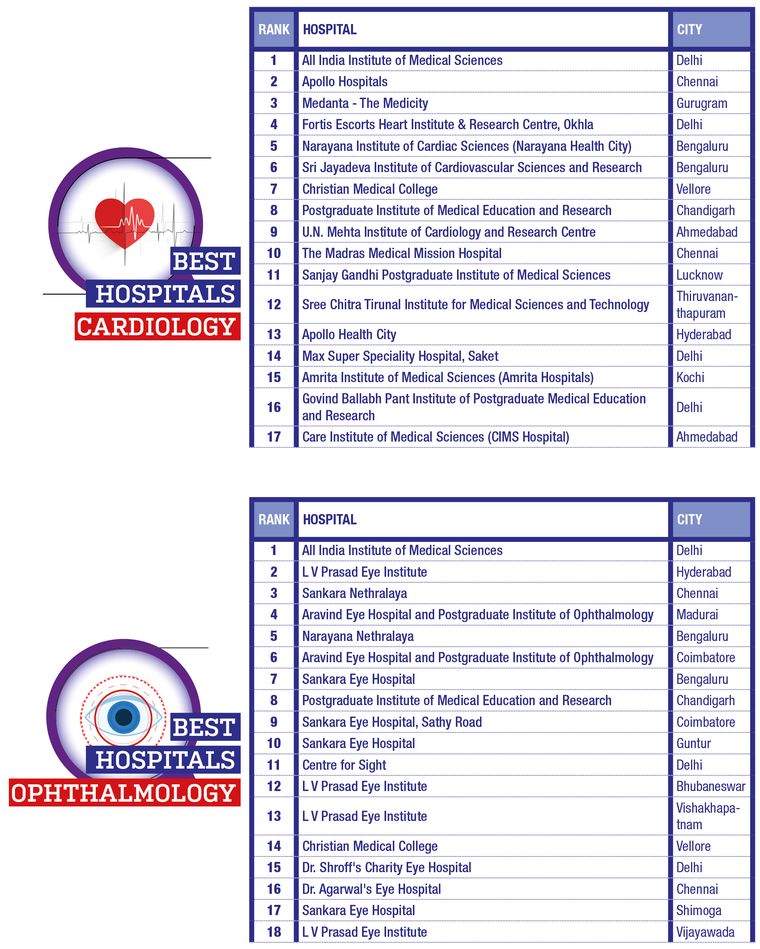
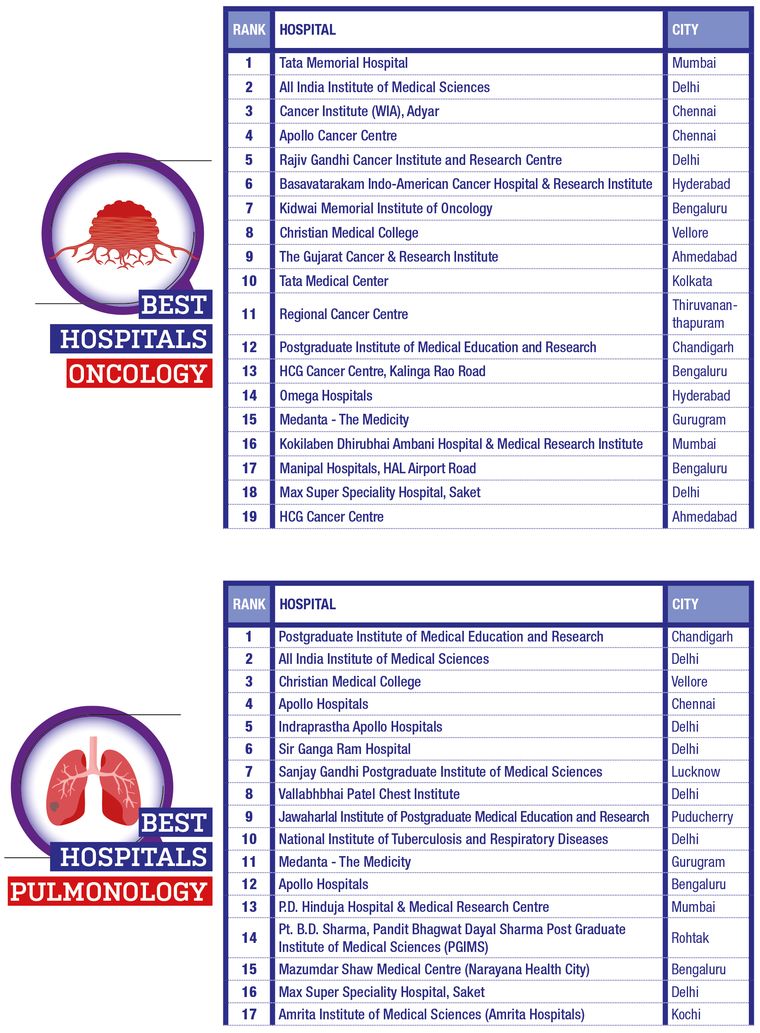
THE WEEK- Hansa Research Best Hospitals Survey 2022
RESEARCH METHODOLOGY
The survey covered 17 cities (plus the National Capital Region) that are important medical centres. Top hospitals for 10 specialisations were also ranked.
PERCEPTUAL DATA COLLECTION
A primary survey was conducted among health care experts―902 general physicians and 1,160 specialists. The sample was selected ensuring proper representation of all cities and specialities.
The experts were asked to nominate and rate the top 10 multispeciality hospitals in India and within their city. Specialists were also asked to nominate and rate the top 10 hospitals for their specialisation. Experts’ response for hospitals they are associated with were ignored.
VALIDATION OF FINDINGS
Data collected from the survey was validated using factual data from hospitals and other secondary sources. The final list was validated by leading doctors. Specialisation rankings were validated by experts who are opinion leaders in their field. City rankings were validated by experts from respective cities.
The core research team conducted telephonic interviews with 80 experts across cities and specialisations to validate the findings.
Also read
- How cancer screening and detection has changed since Covid-19
- How Apollo Cancer Centres are predicting and detecting cancers early
- Exclusive: AIIMS director Dr M. Srinivas on what makes it topper
- How India’s first shoulder-level hand transplant was done
- The art of performing complex surgeries
- Exclusive: Variants unlikely to lead to pandemic, Oxford Vaccine Group director
RANKING METHODOLOGY
The final rank for a hospital is based on the number of nominations received, ranks given, and the ratings on the following five parameters:
•Overall reputation
•Competency of doctors
•Infrastructure and facilities
•Research and innovation
•Patient care
Ranking for a city is based on the perception of the sample surveyed from that city. Hence, the order in city rankings may vary from All India rankings.
Ranking for a specialisation is based on the perception of specialists from that field.
HOW TO USE IT?
The rankings make the opinion of health care experts available to the public. While immense care has been taken to provide an honest assessment, the needs of each patient can be different. So, while this list can be used as a guideline, decisions should be based on what works best for the patient.